Part I can be found here.
When Asline arrived to the Maternity Center around 2:30 on July 15 we had just wrapped up a prenatal visit. We were done with our weekly gig at the government hospital and we were talking about what we all planned to do with our free afternoon.
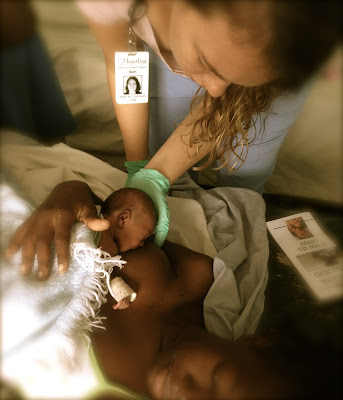 |
| Premature baby girl, born at state-run hospital |
~ ~ ~
Asline walked in to the MC visibly upset and agitated. She had a cousin with her, who waited outside on the porch. Beth McHoul asked several questions in an attempt to gather history, most of which Asline did not verbally respond to at all.
She was having very frequent contractions, the frequency and intensity of her response to the contractions left us thinking she might be 7 or 8cm.
An attempt was made to get all of her vitals. It took a lot longer than we like because when a contraction would come she would pull away and curl inward. She didn't have the ability to cooperate with a blood pressure cuff or a thermometer or a doppler, she was pain-focused. When a contraction came she needed to curl in and rock. Two attempts were made to try and determine how many centimeters she was dilated. Both attempts ended in tears for everyone, she simply couldn't tolerate a typical vaginal exam. KJ had gotten a short chance and thought Asline was about 3cm. We were left without all the information we hoped to have.
For the next hour we attempted with each contraction to calm Asline down, to help her cope, to begin to figure out how one goes about helping a person deliver when they are very uncomfortable with being touched.
Our Maternity Center has standard operating procedures and protocols in place. Those protocols exist to make birth for every woman as safe as it can be. One of the protocols is that every woman has an IV Heplock placed, should she need medicine or fluids in an emergency situation. Getting Asline to cooperate with the placement of the IV heplock was time-consuming and emotionally draining. She did not hold still and it took more than one attempt to get it placed.
Attempts to follow a "labor rest" protocol, thereby helping Asline sleep a few hours failed because she could not allow us to give her morphine via an IM injection.
This photo was taken as we began a conversation with her about a need to transport her. No decision was made at that point, but we wanted to introduce the idea and explain our reasons for considering it.
As we talked and watched Asline continue to lose her mind with contractions we discussed each of our own desires. None of us have ever physically held someone down in order to do our jobs, none of us wanted to be part of doing that. We questioned whether or not Asline would be safe to deliver with us if the baby got into trouble and Asline was unwilling or unable to follow our instructions.
We cried and prayed and posted the picture on Instagram and asked you to pray.
{Side note - When women go into a birth-center or hospital to give birth to their babies, or to attend a gynecological appointment, they expect that the staff there will act in their best interests, that they will receive respectful care and be informed of what is happening. For most women in the developed world (not all) - they can expect their time to be comfortable. They can assume each procedure will be explained fully and with their consent being sought for all actions. Unfortunately, for materially poor women in the developing world, this is not the case. *Many* women leave hospital care having undergone a procedure that was not explained to them, feeling violated and traumatized and possibly even a bit in shock. All that to say, we did not feel right about doing things to Asline that she could not emotionally consent to from her deep place of fear.}
Not more than a half hour after we posted our request for prayer, KJ noted that Asline's baby had flat heart tones. We expect variability and we even expect an early decel here and there, but deceleration late in the contraction is a sign of placental insufficiency, meaning baby is likely being deprived of oxygen rich blood. It was not extremely dangerous, but KJ found the heart tones concerning.
Between our concerns about being forced into a position of being involved in something that made us feel sick, and the heart-tones on the baby, we decided to try a hospital in our area that specializes in high risk OB. We left our Maternity Center hoping maybe we could talk them into considering her as a candidate for a C-Section. Technically speaking, we knew Asline did not fit their acceptance criteria, but we hoped maybe we would run into a sympathetic triage nurse or a kind Doctor. Sometimes, if a hospital is having a particularly slow day, they bend the criteria a little bit.
At the first hospital (run by a large international NGO) Asline behaved as we had seen at our Maternity Center. The nurses said, "Why bring her to us, we cannot do anything if she won't cooperate." Attempts were made to explain to Asline why it was important to try and allow the staff to check her. They failed. We left there defeated.
We were wracking our brains for ideas or alternatives. As we drove out of the parking lot of the first hospital, we decided to go to a hospital next door (a State-run hospital) and see if they might consider taking her for a C/S.
Nirva (pictured above on left) went in to negotiate for care. In Haiti there is no assumption of care. It is always negotiation. Even incredibly difficult situations (way worse than Asline) can be turned away for one reason or another.
Nirva came back out with Asline and said that the hospital agreed that a C-Section would make the most sense with the obvious abuse and trauma in Asline's background. Four Doctors had attempted to check her, she allowed zero of them near her, even kicking one of them twice.
Then another major setback: the Doctor that Nirva spoke with had explained they had no supplies to do a C/S.
We stood in the parking lot deciding if we wanted to go to a private (further away) hospital and ask to pay for C/S or if we wanted to bring supplies to the nearby public hospital. Nirva went in again to clarify with the Doctor and get the list of what the Doctor needed.
He agreed to admit Asline as long as we quickly returned with a huge list of supplies. We left Asline and her cousin and made it back to the Maternity Center as quickly as we could.
Beth McHoul and a few staff members were working with another Mom that had arrived in labor and was already fairly close to delivery. As we drove toward them, they worked to gather all the things on the list.
We checked the supply list, gathered the remaining items, and jumped back in the ambulance to head back through insane Port au Prince traffic to deliver the hundreds and hundreds of dollars in supplies. The Doctor had requested everything from sterile C/S kit to sterile towels to several IV medications for infection, to IV supplies and chux pads. We were basically to provide everything except his trained hands, the Operating Room, and the anesthesia.
I don't know how many years I will need to live here to stop being shocked by this. Apparently more than 9.5 years. I continue to be floored at how little is actually available to the average Haitian person.
I guess if we were to follow suit and try to take this system and embrace it as our own, we could all go open up a Baskin-Robbins franchise. It would be easy, when customers arrive asking for ice-cream to simply tell them, "No, we have *no ice cream* on hand, but if you go get it and bring it to me, along with the scoop and the cone, then I will happily scoop up a nice cone for you and hand it to you."
When we arrived back at the hospital we found out that four doctors had held Asline down to check her. They said she was 6cm and she needed to go outside and walk for an hour and after they did another C/S she would be next person in line.
Beth McHoul sent a message telling us that Nella had delivered a son and all was well at the MC.
KJ and Nirva went to stand outside the operating room with the two huge bags of C/S supplies we brought. Asline walked in the parking lot. We had a teen visitor named Maddie that had come along for the ride and she happily helped Asline walk while I updated the MC on things. I joined Asline and Maddie to walk a bit. The sun was setting by then. I rather appreciate that it sets because you cannot see the rats running along the walls once the darkness fully settles on us. I know the rats are there; don't need to see them.
Asline got tired and I thought I was hearing sounds that matched up with someone ready to start pushing. The area in front of the hospital is very busy with dozens and dozens of people milling around. I did not know where KJ and Nirva were, nor did I know how to find a Doctor or nurse. This is a hospital we rarely go to and I have only been inside once in the last several years. I suggested Asline come lie down on the stretcher and rest in the ambulance. Her hour of walking was only about 20 or 30 minutes in… Once Asline was lying down I asked her if I could check to see where the baby's head was. She said, no and pushed my hand away. On her next contraction I heard the unmistakable sound of involuntary pushing. I asked KJ (by phone) to please come back to the ambulance.
KJ arrived, Asline had a contraction and her water broke all over my legs and feet. I thought "Alright, well, what now?"
Without enough time to really truly decide - we for sure thought the ambulance was better than trying to pass all the people and red tape and get inside the hospital. Asline was contracting again and pushing. It helped us that the ambulance did not really allow her to get totally away from us, she could only push back as far as the back door of the ambulance which was closed and locked. In two pushes (without us touching her until after the head was totally out) she delivered her baby boy. He immediately cried a good strong cry and we were thankful we did not need the bag and mask we had ready should he need help breathing.
KJ had reminded me to be ready for bleeding, as Asline is anemic. It wasn't but 45 seconds later that the blood began gushing. I went in to get the placenta out, the bleeding continued heavily. Together, KJ and I did bi-manual compression. This means that the uterus is being compressed with one hand from the outside and one hand from the inside. It is a horrible, gruesome, life-saving move.
The issue for us was this ... We arrived back at that hospital with supplies for a C-Section. In our minds we had handed our patient off to the hospital. We made a huge mistake (honestly, we will beat ourselves up for this for a long time -- it was very much a stupid stupid mistake on our part) by not being ready for an ambulance hemorrhage. We dug out some money between all the wallets in the ambulance. Nirva ran into the hospital to buy the two medicines we wanted to stop the bleeding while we continued to provide bi-manual compression. She only found one of the two at the hospital and went out into the street to a nearby pharmacy to purchase the second one. Maddie handed us clean towels, and a cord clamp and things we needed for the baby to stay warm.
Several minutes later, maybe 15 or so, Nirva was back and the medicines were delivered. We cautiously removed our hands to see if the bleeding had stopped. Mercifully, it had all but stopped. We could see and feel that Asline was torn and needed repair. We debated whether her blood loss was significant enough to require a transfusion.
After several minutes of focusing only on Asline and baby we saw we had an audience around the ambulance. Time gets weird in those situations, we know the baby was born around 8:30 but I don't know what time we finally looked up at what was going on around our vehicle. The audience included the Doctor that had agreed to do the Cesarean. He angrily asked Nirva why we had not gotten her back inside to deliver. Nirva explained she had been standing outside the OR waiting on him and the Doctor said, "You didn't bring her in to deliver, if you need help now, you're not allowed to bring her back in." This is the guy that told Asline to walk for an hour and then disappeared into a locked room. There are not enough swears in the world for that guy.
Nirva, ever the strong and stoic Haitian nurse, said, "No problem - we've got this."
Once we could see Asline was stable, bleeding was stopped, baby was skin to skin and doing well, we cleaned up the bloodbath as best we could and stepped outside to wash our hands and arms with Maddie's remaining drinking water. A little crowd clapped and said, "Good job. I like it" in broken English. We laughed and said thanks and asked them to pray for Asline.
Once we were back to our kind, loving, calm little Maternity Center house we set everything up to do the repair. Thankfully our protocols include light sedation during a repair when needed. Asline was relaxed a bit via IV meds before her repair was done by Wini.
The next several hours we watched closely to be sure Asline was not showing signs of shock. She nursed her little one and even reached up to hold him with her free hand during the repair.
This morning as we talked to Asline, she shut down, as she is prone to do. Eye contact is difficult, answering questions is difficult. We know not to push her too much.
We shut the door and sat with her, mostly in silent reflection. Occasionally we asked a question or two.
We learned that on Thursday of last week her grandma was involved in a car accident. On Friday her grandma died in a hospital, with Asline at her bedside. On Monday they buried her. On Wednesday Asline went into labor.
We also learned that Asline has more trauma in her past than she can even share.
We knew that though. Her labor and delivery screamed of it.
In the middle of the night, after Asline was tucked into bed with IV antibiotics on board and pitocin dripping into her arm, we finally logged in online and saw all the prayers and comments and intercession that happened for Asline.
To see that hundreds of folks had agreed to pray is truly touching and beautiful to us. I know for sure that Asline couldn't possibly soak that in. Thank you. I don't know why it all went down the way it did, but I do know that Asline and her son are alive and resting in the postpartum room.
I know that love is powerful. If I am being totally honest, I find it hard to believe that it can conquer all, but I am not closed off to that possibility.

Part III of this war is currently being waged.
Will Asline embrace motherhood, will she herself find healing, will this little unnamed baby boy receive every good gift as he deserves? I don't know that yet.
War is long. War is messy.
When this is war, we battle with all the tools we have been given and we wait on miraculous victory.


